(839)
Price range: $26.99 through $54.99
I did end up receiving the item, and honestly it blew away my expectations. The best thiamine products I have ever used. - Stefan
Thiamax, one of the leading thiamine supplements in the US, contains thiamine tetrahydrofurfuryl disulfide (TTFD) making it the perfect natural supplement to improve your thiamine status.
We accept
Free shipping over $250
30-days money back guarantee
In some individuals, thiamine supplements like Thiamax can induce a temporary worsening of certain symptoms such as fatigue, brain-fog, and digestive bloating or gas. These side effects usually last for around one week, and are referred to as the “paradoxical reaction”.
Test results coming soon! They are currently in progress and will be posted as soon as available.
It’s often used for treatment of thiamine deficiency but also useful in supporting energy metabolism, nervous system, and mitochondrial health. This type of thiamine is a highly bio-available form known as TTFD (Thiamine Tetrahydrofurfuryl Disulfide).
Begin with 1 capsule daily, monitor for 2 weeks, then adjust as needed.
1 capsule daily is the standard dose. However, for people who have never taken thiamine supplements or TTFD before, it is best to start with half or quarter of a capsule. This can be done simply by opening a capsule and emptying a portion of the contents into a cold drink or cold food.
Thiamax is best taken in the morning time or early afternoon. If taken in the evening, it may disrupt your sleep cycle.
Either with or without food is fine. The absorption of the supplement is similar either way. Some find it energizing, so try morning first and adjust.
Avoid coffee/tea consumption either 1 hour before or 2 hours after taking Thiamax, as the tannins in these beverages can degrade thiamine.
It might boost energy, so best to take it early. Adjust timing if sleep changes.
Although some people can benefit from taking multiple capsules, it is advised to not go higher than 3-4 capsules without prescription from a healthcare practitioner.
High doses are usually well-tolerated but increase gradually with medical guidance and adjust based on how you respond to it.
Yes, start with 1 capsule and increase/decrease gradually if needed. Consult your healthcare provider for significant changes.
Yes, many do, but consult a healthcare provider for extended use.
Initially some people can experience a “paradoxical reaction”with thiamine supplements. This might include a temporary period of increased fatigue, brain-fog, and poor concentration. These side effects of thiamine supplements usually subside within a few weeks.
Generally, it is advised to supplement Thiamax with 200-400mg of magnesium (in supplemental form) on the same day as Thiamax, and for this we recommend our ThiAssist mineral formula. Likewise, a full-spectrum vitamin B complex is also advised. For this we recommend either our active B complex ThiActive B, or alternatively our methyl-free formula called Thiavite. Please consult with your healthcare provider for specific advice before doing this.
Thiamax uses TTFD (100mg, highly bioavailable) while benfotiamine is less absorbable. Thiamega combines TTFD with other thiamine forms for broader support. See our blog or product pages.
TTFD crosses cell membranes better for quick, effective absorption.
Yes, especially thiamine derivatives like TTFD and benfotiamine can aid in energy production. Many report feeling a lift within weeks.
No, it’s a supplement, not a drug. Some adjust dosages with thiamine, but consult your healthcare provider before modifying prescriptions or adding new supplements.
Some report benefits for various conditions (e.g., clearer thinking, energy, nervous system support), but it’s not a specific treatment. Start low, monitor effects, and consult your healthcare provider for personalized advice.
Generally safe, but consult your healthcare provider to avoid interactions with specific medications.
It supports energy metabolism and pairs well with such diets. Adding magnesium or B vitamins may enhance benefits but be sure to consult a nutritionist for more specific advice.
TTFD’s natural strong odor and sulfur taste are normal. Most get used to it fairly quickly.
95% of our customers say they would recommend Objective Nutrients

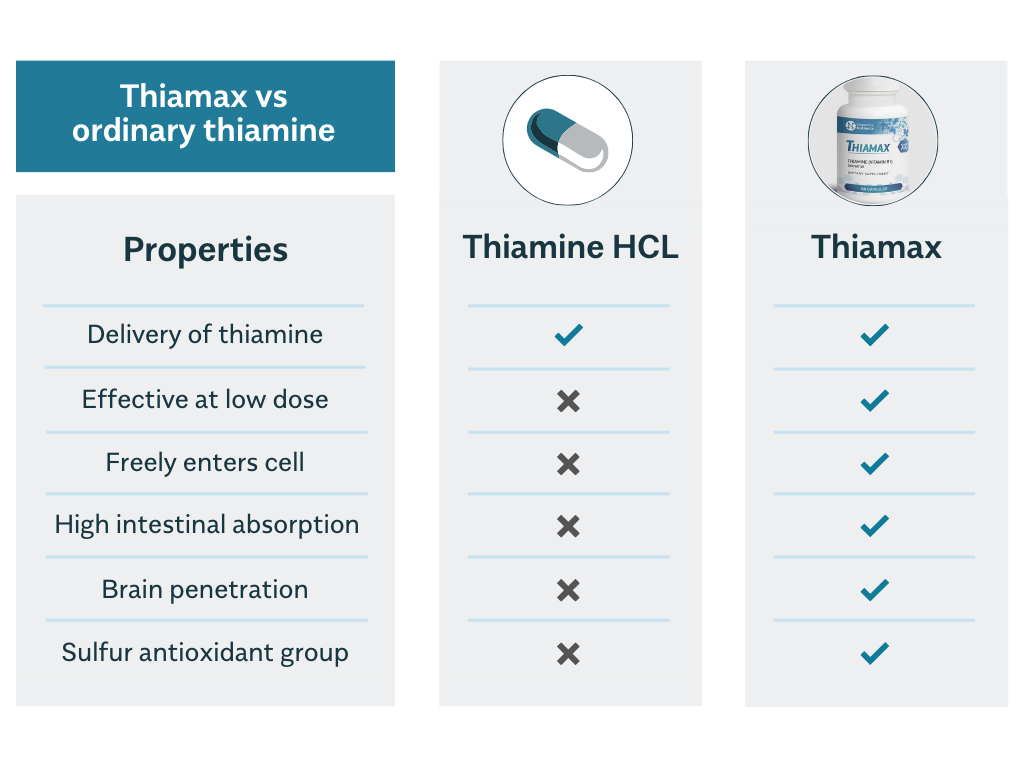
Thiamax, a synthetic thiamine supplement, contains a highly-bioavailable derivative of thiamine (vitamin B1) called TTFD – thiamine tetrahydrofurfuryl disulfide. This form has been widely researched in Japan for its therapeutic potential in addressing thiamine deficiency.
Unlike ordinary forms of Vitamin B1 or thiamine supplements, TTFD’s molecular structure allows it to pass through intestinal and cellular membranes without the requirement for a transport system. Once inside the cell, it can be activated and used as a cofactor in important biochemical processes.
TTFD also has a demonstrated capacity to penetrate the blood brain barrier and increase thiamine levels in the brain and central nervous system, where it may be used to support optimal cognition and maintain autonomic nervous system function.
Due to its superior bioavailability, TTFD can be taken in much lower doses than what is considered the “therapeutic dose” of other forms such as thiamine salts. Thiamax also contains a small amount of magnesium (as magnesium taurate), which is a mineral that is important for supporting how cells can utilize thiamine, making it a useful way to supply thiamine to the body and improve thiamine status.
Also, what makes Thiamax superior to other Thiamine supplements is the fact that it’s the only form of TTFD in the world that doesn’t use any artificial fillers or excipients.
Elliot Overton is a nutritionist based in France, and is considered to be an expert in the clinical application of high-dose thiamine therapy.
He frequently lectures and speaks at educational events aimed at practitioners, helping to broaden the understanding and application of thiamine in clinical settings. He is co-founder and CEO of Objective Nutrients, a nutraceutical company specialising in excipient-free thiamine derivatives and related supplements.
